Contact us today for a consultation with one of our physicians.
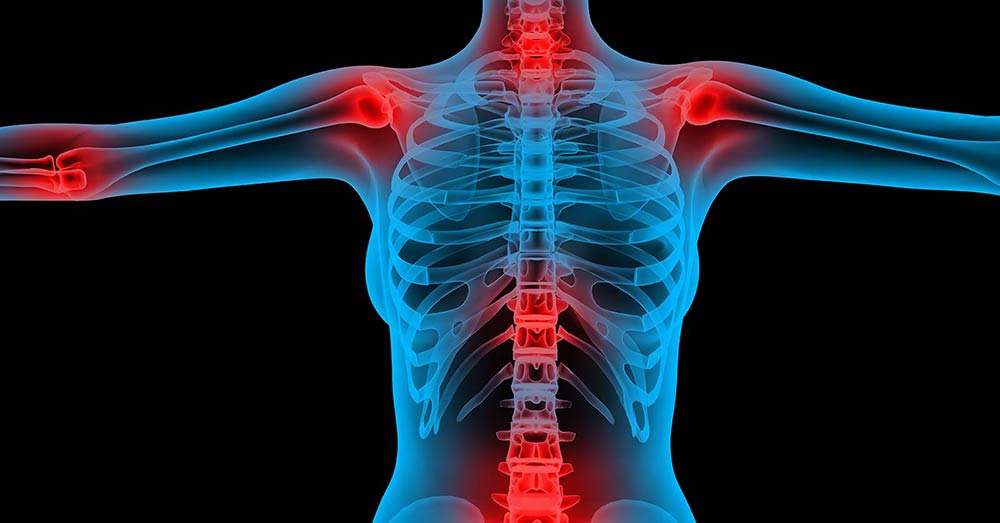
Epidural injections are used to treat pain that starts in the spine and radiates to an arm or leg. Arm or leg pain often occurs when a nerve is inflamed or compressed ("pinched nerve").
Epidural injections involve injecting an anesthetic and an anti-inflammatory medication, such as a steroid (cortisone), near the affected nerve. This reduces the inflammation and lessens or resolves the pain. This type of epidural injection is a therapeutic one.
For diagnostic purposes, an epidural spinal injection can be done at a very specific, isolated nerve to determine if that particular nerve is the source of pain. Sometimes only an anesthetic is injected. The immediate response to the injection is closely monitored. If the pain is completely or nearly completely relieved, then that specific nerve is the primary cause of the pain symptoms. If there is little pain relief, then another source of pain exists.
Facet joint injections can also be done for both diagnostic and therapeutic reasons.
These types of injections are often used when pain is caused by degenerative/arthritic conditions or injury. They are used to treat neck, middle back, or low back pain. The pain does not have to be exclusively limited to the midline spine, as these problems can cause pain to radiate into the shoulders, buttocks, or upper legs.
For diagnostic purposes, facet joints can be injected in two ways: injecting anesthetic directly into the joint or anesthetizing the nerves carrying the pain signals away from the joint (medial branches of the nerve). If the majority of pain is relieved with anesthetic into the joint, then a therapeutic injection of a steroid may provide lasting neck or low back pain relief.
If anesthetic injections indicate that the nerve is the source of pain, the next step is to block the pain signals more permanently. This is done with radiofrequency ablation, or damaging the nerves that supply the joint with a "burning" technique.
Sacroiliac joint (SI joint) injections are similar to facet joint injections in many ways. The SI joints are located between the sacrum and ilium (pelvic) bones.
Problems in the SI joints have been shown to cause pain in the low back, buttock, and leg. Typically, one joint is painful and causes pain on one side of the lower body. It is less common for both SI joints to be painful at the same time.
This joint can also be injected for both diagnostic and therapeutic purposes. Anesthetizing the SI joint by injection under X-ray guidance is considered the gold standard for diagnosing SI joint pain. A diagnostic injection of the sacroiliac joint with anesthetic should markedly diminish the amount of pain in a specific location of the low back, buttock, or upper leg.
A therapeutic injection will typically include a steroid medication, with the goal of providing longer pain relief.
For more information about the types of therapeutic injections we offer patients in the Los Angeles and Beverly Hills, CA area, for spinal pain management, please contact us at 855-SOMA-844 (855-766-2844).
A spinal cord stimulator is an implanted device that sends electricity directly into the epidural space, around the spinal cord, to relieve pain. This procedure is offered to patients when non-surgical treatment does not provide efficient pain relief. It may be indicated for patients who have back pain, post-surgical pain, injuries to the spinal cord, nerve pain, and more. There are thin wires that are placed in the epidural space and a generator that provides the battery. Patients have a remote control that allows them to stimulate electrical impulses when they are feeling pain.
This procedure is done in two parts: first a trial and then the implantation. Both procedures occur in the OR. During the trial, the surgeon will use x-ray to insert a temporary device. For about a week, the patient will determine how well the device reduces their pain. If unsuccessful, the temporary device can be easily removed in the clinic. If successful, a surgery may be scheduled to permanently implant the device. Patients are able to leave the same day as their procedure. There may be some soreness at the incision site. The doctor will discuss a medication regimen with the patient for recovery, if necessary. Usually, the patient may resume regular activity typically 1-2 weeks after the procedure.
This procedure is commonly covered by Medicare and most major policies. Of course for the procedure to be covered by insurance, first most conservative measures have to be exhausted. Many policies require a prior authorization for the procedure to be done. Some policies have a deductible, copay or coinsurance which might be due at the time of the surgery and or after the procedure is performed.